|
Beating Heart: a patchwork of pieces from the recent literature |
|
Background
1947 Vineberg Mammary artery implant into cardiac
muscle.
CPB
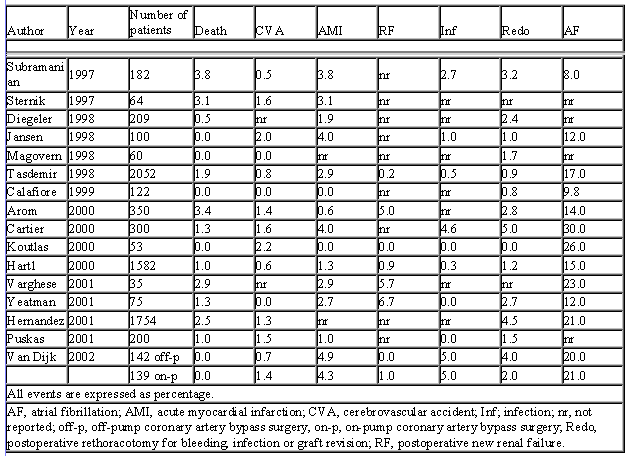
Off-pump Clinical results Hemodynamic changes Positioning When the circonflex or right coronary artery needs to be grafted a nearly vertical displacement may be needed. It could be surprisingly well tolerated in most patients, but can provoke a significant drop in blood pressure and myocardial flow (specially with patients with left ventricular hypertrophy or poor ventricular blood pressure) 17 Heart manipulation during OPCAB may cause hemodynamical instability in particular for access to the posterior and lateral walls. The “no compression” technique involves enucleation of the heart without any compression on the cavities, and stabilization of the target area with a suction device. In order to analyse a homogenous group, 26 consecutive patients with triple grafts, one to each side of the heart in the same sequential order (posterior, lateral and anterior wall successively) selected. A coronary shunt used for all the anastomoses. Heart rate, mean pulmonary arterial pressure, pulmonary capillary wedge pressure, mean arterial pressure, cardiac output index, and central venous saturation were monitored. None of the hemodynamical parameter differed significantly from baseline value for all three territories. While hemodynamics was perfectly maintained during the posterior and anterior walls revascularization, exposure of the lateral wall led to marginal changes only 18. During off-pump surgery, with multiplane intraoperative echocardiography, the mitral annulus at end diastole was reconstructed in the different positions and correlated with hemodynamic changes. Significant distortion of the mitral annulus with enlargement of the left atrium and pulmonary veins was demonstrated, which correlated with high left atrial pressures19 Surgical exposure by anterolateral thoracotomy showed no significant hemodynamic changes. Through sternotomy, stroke volume was significantly reduced by dislocation at all target sites: by 6% at the left anterior descending artery, 25% at the diagonal branch artery, 14% at the right coronary artery and 21% at the obtusemarginal artery. The application of head-down positioning increased not only surgical exposure but also preload, producing correction of ventricular filling pressures and output. In a minority of cases, dopamine was added to maintain baseline hemodynamic values.20 Intracoronary shunts Forty patients were randomized to off-pump with a shunt (n=20) or with the proximal coronary occluded by a soft snare (n=20). Hemodynamic measurements were recorded at base line, during construction, and after completion of each distal anastomosis. Grafting of the left anterior descending coronary anastomosis was associated with a significant decrease in stroke volume, cardiac index, and mean arterial pressure and an increase in pulmonary capillary wedge pressure and systemic vascular resistance in the snare but not in the shunt group. During grafting of the posterior descending coronary artery there was a marked decrease in stroke volume and cardiac index, and an increase in central venous pressure in both groups, and an increase in heart rate, mean pulmonary arterial pressure, pulmonary capillary wedge pressure, and systemic vascular resistance only in the snare group. The most extensive changes were observed during the circumflex coronary artery anastomosis with a reduction in stroke volume, cardiac index, and mean arterial pressure and an increase in central venous pressure, pulmonary wedge pressure, pulmonary arterial pressure, and systemic vascular resistance in both groups. In all settings, these changes were transient and recovered once the heart was returned to its anatomical position in the shunt group, whereas stroke volume and cardiac index remained reduced, and systemic vascular resistance was elevated in all settings in the snare group.21 Hemodynamic changes were recorded at the completion of the anastomosis before release coronary snaring and stabilization and compared to baseline. Conclusion: Manipulation of the beating heart during OPCABG surgery brings significant fluctuations in the patients’ hemodynamics. Mean PAP increase and cardiac output index drop were more significant during manipulation of the anterior territories suggesting a more severe diastolic restrictive disease during anterior wall manipulation 22 Methods: 2D transoesophageal echocardiography was used to derive systolic wall motion indices and pulsed Doppler parameters of diastolic function. A continuous cardiac output thermodilution pulmonary artery catheter was used to provide hemodynamic measures of left ventricular function. Data was obtained prior to, during and following coronary grafting. Specially during circmflex grafting, waal motion score index was significantly increased when compared to right coronary grafting and left anterior descending artery grafting. All functional parameters returned to baseline by the end of surgery.23 Surgical complications Injury to the pulmonary vein during placement of deep pericardial sutures and postoperative infusion heparin were the likely causes of this rare but potentially fatal complication (retropericardial hematoma) of an off-pump bypass operation. 24 We describe an unusual development of a large retropericardial hematoma following otherwise uneventful beating heart coronary surgery25 We report here an unusual complication of an intramyocardial dissecting hematoma with an epicardial rupture caused after using the Octopus 3 stabilizer 26 Technical aspects In off-pump coronary artery bypass surgery, heparin should be reverted with protamine, otherwise the postoperative bleeding risk might increase. Part heparin reversal might not increase postoperative bleeding risk, but it may reduce dose-dependant protamine adverse effects.27 High thoracic epidural anesthesia allows earlier extubation compared with the opioid anesthesia technique (0.9 versus 4.5 hours). Perioperative management and the incidence of postoperative complications did not differ between anesthetic techniques. Major complications, such death, intraoperative myocardial infarction, and stroke, did not occur.28 Intraoperative coronary angiography confirms graft patency with the possibility to revise graft failure. A total of 57 grafts in 45 patients who underwent off-pump coronary bypass operations were included. Follow-up angiographies were performed at 3 months and at 12 months. The most frequent finding in on-table angiogram was spasm, which was not present at follow-up. Out of kinks, only one developed into a significant stenosis at follow-up. Of 44 grafts that were normal on-table, 37 (84%9 were normal at the follow-up. 11 grafts with significant lesions on-table, eight (73%) were normal at the follow-up. Conclusion: On-table angiograms can be occasionally difficult to interpret because not all findings are important for later patency. Optimal results on-table predict good long-term results with a negative predictive value of 0.84, whereas significant lesions on-table have less impact on the follow-up results because the positive predictive value was only 0.3829 The results demonstrated that graft anastomosis by power Doppler imaging correlate well with the angiographic measurements. High-frequency epicardial echocardiography can provide meaningful information on the target coronary artery, and power Doppler imaging can accurately measure graft anastomoses and can detect technical errors and inadequacies during coronary artery bypass grafting without cardioplulmonary bypass30. Combined off-pump coronary bypass grafting and carotid endarterectomy is a safe and effective procedure31,32 General population17 In-hospital and 30 day clinical events after off-pump bypass surgery
A review of two large databases employed by multiple surgeons in the hospital of two institutions identified 8,758 multivessel CABG procedures performed from January 1998 to July 2000…. Procedures were also divided into two treatment groups based on the use of cardiopulmonary bypass (CPB): 6,466 had CABG with CPB and 1,983 had CABG without CPB. On-pump CABG was associated with increased mortality compared with off-pump CABG by univariate analysis, 3.5% versus 1.8%, despite a lower predicted risk in the on-pump group. CPB was associated with increased mortality by multiple logistic regression analysis….Elimination of CPB improves early survival in multivessel CABG patients. Rigorous attempts to statistically account for selection bias maintained a clear association between CPB and increased mortality33 Between 1998 and 2000, 1,741 off-pump CABG and 6,126 on-pump CABG procedures were performed. This study showed that patients having off-pump procedures are not exposed to a greater risk of short term adverse outcomes. These data also provided evidence that patients having off-pump CABG have significantly lower need for intraoperative and post operative intraaortic balloon pump, lower rates of postoperative atrial fibrillation and a shorter length of stay.34 Off-pump CABG surgery is associated with less morbidity and mortality and accelered recovery compared with on-pump CABG surgery. Off-pump CABG may represent the ideal revascularization strategy for patients at high risk35 Early mortality was off-pump group: 0.83%, on-pump: 2.83% (difference not being statistically significant). The incidence of post-op stroke (1.66% / 3.66%), renal failure (2.5% / 5.66%) and gastrointestinal complications (1.66% / 1.21%) was likewise not significantly different in the two groups. However, the off-pump patients had a statistically significant lower incidence of low cardiac output (43.3% / 29.5%), atrial fibrillation (11.66% / 30.36%), blood product transfusion (39.66% / 89.87%), time on ventilator (5.96hr / 10.31hr), and post-op hospital stay (7.79d / 9.81d). Medium term results (recurrence of angina, late mortality, cardiovascular events, and need for revascularization) were similar in the two groups 36 From March 1997 to November 1999, we randomly allocated 200 patients to off-pump and 201 to on-pump coronary surgery. Off pump coronary surgery significantly lowers in hospital morbidity without compromising outcome in the first 1-3 years period after surgery compared with conventional on-pump coronary surgery37 A group of 500 patients who were consecutively operated on cardiopulmonary by-pass and a group consisted of 506 patients who were consecutively operated on using “off pump” techniques. Preoperative risk profile in both groups were similar as was as in the operation time. There was distinct benefit in amount of homologous transfusion, period of ICU stay, increased usage of radial artery conduit and improvement of in transoesophageal echocardiography assessment of ischaemic mitral incompetence immediately after revascularisation in off-pump group. Though there was a lower mortality in the off pump group (i.e. 3/50 vis-a-vis 10/500 in on-pump group) this is not of statistical significance. Improvement in left ventricular ejection fraction>5.0% occured more frequently in one month follow-up visits of the off-pump group patients. Period of return to active life was also shorter (28 versus 56 days) 38 OPCAB (1 vessel) incurs no increased risk of in-hospital mortality. In contrast, there is a significant reduction in morbidity in patient undergoing OPCAB when compared to that performed on cardiopulmonary bypass39 From May 1997 to November 2000, 1,843 consecutive patients underwent isolated myocardial revascularization. From this total, 919 patients were done without CPB and 924 were done with CPB. Patient that converted from without CPB to with CPB were included in group without CPB. Thirty-three variables were evaluated with univariate and multivariate analysis to identify the independent variables predictive of higher incidence of early mortality, acute myocardial infarction, cerebrovascular accident, and early major events. Results. Early mortality was 2.2% (off-pump 1.4%, on-pump: 3.0%; p=0.016), acute myocardial infarction incidence was 1.8% (off-pump: 1.1%, on-pump:2.6%; p=0.027), cerebrovascular accident incidence was 0.9% (off-pump: 0.8%, on-pump: 1.0%; p= not significant), and early major events incidence was 6.7% (off-pump:5.3%, on-pump: 8.2%; p<0.001). Stewise logistic regression analysis showed that CPB was an independent risk factor for higher mortality, higher incidence of acute myocardial infarction and higher incidence of early major events.40 Between June 1, 1991 and September 30, 2001, a total of 1089 patients with three vessel disease underwent on-pump CABG. After 1997, a total of 310 patients with three-vessel disease underwent off-pump CABG. The 2 groups were age and gender matched. Significant comorbidities were more often observed in the off-pump group than in the on-pump group. The mean number of bypass grafts in the off-pump versus on-pump CABG was 3.3 vs 3.7. The mean intubation period: 7.9 vs 11.7 hours, intensive care unit stay: 2.2 vs 3.0 days, and postoperative hospital stay: 14.5 vs 17.5 days. In hospital mortality rate (0.6% vs 1.2%) and morbidity rates (10.3% vs 12.9%) were not significantly different. After surgery, calculated event-free rates at 2 years were 93.3% vs 91.9% (P = not significant)41 The optimal combination of arterial grafts for quadruple coronary artery bypass is the bilateral internal mammary artery, the radial artery, and the gastroepiploic artery. Patients who underwent quadruple bypass in our hospital group between December 1995 and March 2001 were retrospectively analyzed to determine whether off-pump surgery (n=27) provides better outcomes than conventional on-pump surgery (n=51). Preoperative risk factors as well as the mean number of distal anastomosis (4.5 in the off-pump versus 4.8 in the on-pump patients) were not significantly different between the 2 groups. Postoperative recovery was significantly faster in the off-pump group than in the on-pump group (intubation time: 6.4 versus 16 hours; stay in intensive care unit: 2 versus 3 days; and postoperative hospital stay: 12.3 versus 15.8 days). Early free graft patency rates did not differ significantly (90.3% versus 89.3%). No late cardiac events were observed in the off-pump group, while 4 occurred in the on-pump group42 Myocardial revascularization without CPB using arterial conduits can be accomplished with the same quality of results obtained with the use of CPB.43 High-risk patients. Fifty-seven multivessel disease OPCABG patients had markedly increased Parsonnet scores. The average ejection fraction of the patients was 42% (+/- 12.3) and their age ranged from 52 to 85 years. Unstable angina was present in 42 patients (74%) and 10 patients underwent OPCABG within 24 hours of the occurrence of acute myocardial infarction. In addition to severe coronary artery disease 32% of the patients presented with congestive heart failure, insulin-dependent diabetes (18%), renal failure (22%), peripheral vascular disease (18%), and neurologic disorders (14%). An average of 2.6 +/- 0.9 grafts/patient were performed and the posterior descending artery or marginal branches of the circumflex artery or both were grafted in 90%. The mortality rate was 3.5%44 The purpose of this study was to provide a comparison of the early and long term outcome between patients groups with left dysfunction (LVEF <40% or LVPS > or = 15) operated with or without cardiopulmonary bypass. All patients received one vessel bypass left internal mammary artery to left descending artery. In spite of more than four times as many patients in the cardiopulmonary bypass group requiring inotropic support after surgery, survival and cardiac death were similar for both groups. Off-pump bypass surgery conserves the blood constituents. The benefits of both techniques to improve the left ventricular performance score and ejection fraction were similar, but postoperative extubation time, length intensive care unit and hospital stay were reduced significantly in the beating heart group 45 From April 1996 to December 2000, clinical data for consecutive patients undergoing coronary artery revascularization were prospectively entered into a database. Data were extracted for all patients considered to be high risk, defined as the presence of one or more of ten adverse factors. Unadjusted odds ratios for intensive care unit or high-dependency unit stay, total length of stay, blood loss of more than 1000ml, postoperative hemoglobin and transfusion requirement all showed a highly significant benefit for the off-pump group. After adjustment for prognostic variable odds ratio remained essentially unaltered except for blood loss of more than 1000ml. Sensitivity analyses confirmed the robustness of these findings.46 Between January 1997 and December 2000, 355 355 patients with LV dyfunction (EF equal to or less than 30%) underwent off-pump coronary bypass surgery. During the same period, 959 patients with LV dysfunction underwent coronary artery surgery on cardiopulmonary bypass. The mortality was 3.9% and 6% in off pump and on-pump respectively. Post-operative morbidity was less for off pump group but it was statically significant in incidence of atrial fibrillation and prolonged ventilation which were low in off-pump group. The hospital stay was significantly less in patients operated off-pump.47 Age greater than 80 years, reoperative CABG, a left ventricular ejection fraction percentage less than 40%: These three subgroups were compared according they were operated on- or off-pump. Free from overall complications was significantly higher (p<0.005) in the off-pump group. Actual mortality rates in the off- and on-pump groups were comparable.48 Medical records of patients undergoing off-pump CABG (n=126) were retrospectively reviewed. We classified them into two subgroups: low risk (EuroSCORE <5, n=72) and high risk (EuroSCORE >5, n=54). EuroSCORE high risk patients showed significantly higher rates of blood transfusion (70 vs 31%; p=0.0001), intraaortic balloon pump insertion (16 vs 3%; p=0.013), atrial fibrillation (43 vs 22%; p=0.014), and renal failure (13 vs 3%9; p=0,028). ICU length of stay was significantly longer in the high risk group (25 vs 22hours; p=0.002). There was also a higher perioperative mortality in the high risk group () vs 0%; p=0.008).49 Elderly patients From April 1996 to December 2000, data of 3842 patients undergoing coronary revascularisation were prospectively entered into a database. Data were extracted for 990 patients older than 70 years (219, 22,1%, with off-pump surgery). After adjustment for prognostic variables, off-pump surgery was found to be associated with reduced inotropic use, intra-operative arrythmias, blood loss and transfusion requirement when compared to on-pump coronary surgery. Mid-term mortality or cardiac-related events were similar in the two groups50 This retrospective, nonrandomized study consisted of 1,872 patients 70 years of age and older. Of these, 1389 underwent CABG with CPB and 483 patients without. At univariate analysis, patients in the off-pump group had higher rate of freedom from complications (82.2% versus 81.3), a lower incidence of stroke (2.1% versus 4.2%9 than patients in the CPB group. The risk adjusted mortality in the off-pump group was lower (1.9% versus 2.1%). Multivariate analysis showed that while the use of CPB correlated independently with an increased risk of overall complications, it was not associated with a higher probability of death or stroke.51 In this study, we investigated the efficacy of off-pump CABG for patients aged 75 years or more. Intubation time ((.4 versus 18.4 hours), intensive care unit stay (2.2 versus 3.5 days), and postoperative stay (13.8 versus 22.2) days were significantly shorter in the off-pump group than in the on-pump group(p<0.05). The frequency of the occurrence of major complication was significantly lower in the off-pump group than in the on-pump group, especially in regard to postoperative stroke and respiratory failure. Multivariate analysis showed that off-pump CABG significantly reduced patient recovery period and the incidence of postoperative complications. Early follow-up results, cardiac event-free and survival rate did not significantly differ between the two groups.52 Registry data and patients’ notes and charts were reviewed for 56 elderly off-pump CABG patients (age 78.5 +/-3.5 years) and 87 consecutive on-pump CABG patients (age 77.2+/-2.4 years). The length of stay in the intensive therapy unit was 35.4 +/- 52.9 hours for off-pump CABG and 77.6 +/- 144.9 hours for on-pump CABG patients (p=0.0008). No patient died within 30 days in the off-pump group, while 9 (11%) on-pump patients (p=0.0066) died within 30 days. The incidence of serious complications (including pulmonary oedema, septcaemia, permanent stroke and renal dysfunction requiring haemofiltration or haemodialysis) was one (2%) in the off-pump group and 11 (13%) in the on-pump group (p=0.028). Ten (12%) of intra aortic balloon pumps were inserted in the on-pump group compared to only one patient (2%) in the off-pump group (p=0.05). Nine (11%) on-pump patients were re-operated on for bleeding compared to no off-pump patient needing re-operation (P=0.011). 53 Chart and provincial cardiac care unit registry data were reviewed for 30 consecutive elderly off-pump CABG patients (age 74.9 +/- 4.2 years) and 60 consecutive on-pump CABG patients (age74.9 +/- 4.1 years) with similar risk factors profiles. Mean hospital stay was 6.3 +/- 1.8 days for off-pump patients and 7.7 +/- 3.9 days for on-pump patients (p<0.05). Average intensive care unit stay was 24.0 +/- 10.9 hours for off-pump patients versus 36.6 +/- 33.5 hours for on-pump patients (p<0.05). Atrial fibrillation occured in 10.0% of off-pump patients and 28.3% on-pump patients (p<0.05). Low output syndrome was observed in 10% of off-pump patients and 31.7 of on-pump patients (p<0.05).Cost was reduced by $1,082 (Canadian) per patient in the off-pump group.54 In patients aged 70 years and older, multivessels off-pump surgery is associated with lower rates of postoperative atrial fibrillation and reduced transfusion requirements.55 Patients in the beating heart group were older (75 +/- 4 vs 74 +/- 3, p=0.001). Gender distribution and other preoperative risk factors were comparable for the two groups. On average, 3.0 +/- 0.8 and 2.8 +/- 0.7 grafts per patient were completed in the off-pump and the on-pump groups respectively (p=0.007). Perioperative rates (off-pump: 3.1%, on-pump: 3.6%), perioperative myocardial infarction (off-pump: 2.0%; on-pump: 5.1%) and neurologic events (off-pump 1.0%, on-pump 3.2%) were comparable for the two groups. The incidence of postoperative atrial fibrillation was lower in the off pump group (42 vs 54%, p=0.05). The need for allogenic blood transfusions was significantly less in the off-pump group (53 vs 82%; p=0.001).56 Graft patency With respect to graft patency, data from observational studies in comparison with historical controls suggest similar early graft patency between off-pump (91-99%) and on-pump (94-99%) bypass surgery 57,58 We analyzed the results of 122 consecutive off-pump CABG cases compared with those of 65 consecutive on-pump with cardioplegia CABG cases and those of 19 consecutive on-pump beating CABG cases. The patency rate of saphenous vein grafts after off-pump CABG was significantly lower than that of arterial grafts in the early postoperative coronary angiography, and was also significantly lower than those of saphenous vein grafts of on-pump groups (with or without cardioplegia) in the postoperative 1-year coronary angiography,, altough there was no significant difference in 1-year patency of arterial grafts among the three groups. Our data suggest that a specific perioperative anticoagulant therapy may be advisable in patients undergoing off-pump CABG with saphenous vein grafts59. Neurological events Only one study conducted at the University Medical Center Utrecht, using the Octopus Tissue Stabilizer, directly compared off- and on-pump bypass surgery by means of a randomized clinical trial 60,61. This study revealed no superiority in 30 day clinical outcome and only a modest superior cognitive outcome at three months which became negligible at 12 months after off-pump surgery. There was a reduced need for blood products in the off-pump group, and there was a 41% reduction in postoperative creatine kinase MB release. Logistic regression analysis did not show that cardiopulmonary bypass was a risk factor for either surgical mortality or stroke 62 During the study period, 4,077 patients underwent CABG and of these 923 (22,6%) had off-pump surgery. Forty-five patients suffered a perioperative stroke (1,1%). Multivariate regression analysis identified several preoperative fact as independent predictor of stroke, i.e., age, unstable angina, serum creatinine greater than 150 mcg/ml, previous cerebrovascular accident, peripheral vascular disease and salvage operation. When operative risk factors were added to the adjusted model, off-pump surgery was associated with a substantial, but not significant, protective effect against stroke63 The incidence of focal neurologic deficit was 1.6% in the on-pump group, 0,4% in the off-pump with aortic manipulation group, and 0.5% for the off-pump without aortic manipulation group. The results of the multivariate logistic regression analysis demonstrated that use of CPB was a risk factor for focal neurologic deficit64. The incidence of postoperative stroke was 0.3% in the off-pump group and 2.0% in the on-pump group. Multivariate analysis demonstrated that the use of cardiopulmonary bypass, age over75 and peripheral vascular disease were isolated predictors of postoperative stroke. Conclusion: The incidence of postoperative stroke was lower in the off-pump group than in the on-pump group, even though the side-clamp was applied to the ascending aorta for aortocoronary bypass. The use of side clamping for off-pump aorto coronary bypass does not increase the risk of postoperative stroke65. Patients undergoing on-pump coronary bypass grafting were 1.8 times more likely to suffer a stroke postoperatively than OPCAB patients after controlling for preoperative risk factors through matching. Independent predictors of stroke identified from the multiple logistic model included on-pump operation (versus OPCAB operation), female gender, 4 to 6 vessels grafted (versus <4 grafts), hypertension, history of previous cerebrovascular accident, carotid artery disease, chronic obstructive pulmonary disease, and depressed ejection fraction 66 Heart damage The off-pump CABG group demonstrate a significant reduce Troponin T release profile compared with the on-pump CABG group.67 A significant reduction of the cardiac cell damage was observed in the off-pump CABG group versus the on-pump group over time in the absence of acute myocardial ischemia or infarction. In addition, systemic and myocardial lipid peroxidation as measured by the malondialdehyde levels are lower in the off-pump group when compared to on-pump. Finally, plasma levels of big-Endothelin significantly rose in the on-pump group but not in the off-pump group. Conclusion: The data of the present study indicate that CABG without the use of CPB and cardioplegic arrest reduces myocardial cell damage and lipid peroxidation. It is also associated with a reduced activation of the potent vasoconstrictor peptide endothelin.68 Atrial fibrillation Avoid CPB does not seem to reduce the incidence of postoperative AF in CABG surgery69 Renal impairment Although renal complication or serum marker of kidney dysfunction were absent, sensitive indicators revealed significant injury to renal tubules and glomeruli following either off-pump or on-pump coronary surgery. These results suggest that avoidance of cardiopulmonary bypass does not offer additional renoprotection to patients at low risk of perioperative renal insult during CABG70 We found that off-pump coronary revascularization induced significantly less changes in microalbuminuria, fractional excretion of sodium, free water clearance, N-acetyl-beta-D glucosaminidase, and free hemoglobin as compared with operations with CPB. Markers returned to baseline within 2 days after the operation. Off-pump coronary surgery attenuates transient renal injury compared with on-pump coronary artery bypass grafting.71 Isolated CABG was performed on 40 hemodyalisis patients between September 1993 and December 2000. Among them, off-pump CABG was performed in 16 and on-pump CABG in 24. Blood transfusion was significantly less frequent in the off-pump group than in the on-pump group. Postoperative complications were more frequently observed in the on-pump group (7,1% off-pump vs 25.0% on-pump). There were two hospital deaths in the on-pump group and none in the off-pump group. Postoperative intubation time, ICU stay, and hospital stay were significantly shorter in the off-pump group than in the on-pump group. Although follow-up period was short (1.1+/-0.7 years), no cardiac events occured in the off-pump group72 From June 1996 to December 1999, data of 3,250 consecutive patients undergoing coronary artery bypass grafting were prospectively entered into the Patient Analysis & Tracking Systems (PATS, Dendrite Clinical Systems). Two hundred and fifty-three patients with preoperative serum creatinine more than 150 micromol/L were identified (202 patients on-pump, 51 patients off-pump) and clinical outcomes were analysed. Conclusion: This study suggests that off-pump coronary artery bypass operations reduce in-hospital morbidity and the likelihood of acute renal failure in patients with preoperative nondialysis-dependant renal insufficiency undergoing myocardial revascularization.73 Blood impairment. Conventional cardiopulmonary bypass (CPB) surgery increases the iron loading of plasma transferrin often to a state of plasma iron overload, with the presence of low molecular mass iron. Such iron is a potential risk factor for oxidative stress and microbial virulence. Patients undergoing beating heart surgery had significantly lower levels of plasma non-haem iron, and a decreased percentage saturation of the transferrin at all time points compared to conventional bypass patients. Beating heart surgery appears to decrease red blood cell haemolysis, and tissue damage during the operative procedures and thereby significantly decreases the risk of plasma iron overload associated with conventional bypass.74 Inflammatory response Twenty patients undergoing coronary operation with CPB were studied. Patients undergoing off-pump coronary bypass and healthy subjects served respectively as stressed and normal groups. Spontaneous apoptosis was significantly delayed in polymorphonuclear leukocyte from CPB patients when compared with either the stressed or control patients. Conclusion: Inflammatory mediators during CPB prolong the functional lifespan of neutrophils through modulation of apoptosis, and potentiate the inflammatory response observed after coronary bypass operation.75 Cardiopulmonary bypass (CPB) and operative trauma are associated with increased expression of proinflammatory mediators. We determined the relative contribution of CPB on activation of cytokines and adhesion molecules in patients undergoing coronary revascularization by comparison them with patients receiving off-pump coronary artery bypass grafting. Both systemic and endomyocardial expression of adhesion molecules were lower in the off-pump group. Coronary revascularization with CPB resulted in a significant higher expression of TNF-alpha, which was associated withP-selectin and ICAM-1 expression. This was accompanied with higher catecholamine requirement in the on-pump group in the early postoperative period. Despite comparable surgical trauma, the off-pump procedure without the use of CPB and cardioplegic arrest significantly reduces systemic and cardiac adhesion molecule expression and catecholamine requirement.76 Endothelial dysfunction Fourteen patients operated off-pump were compared with 21 patients undergoing conventional CABG with CPB. The indexed pulmonary vascular resistance was measured before and during an infusion of acetylcholine in the pulmonar artery. Twelve patients operated on-pump received saline instead of acetylcholine. Before surgery pulmonary vascular resistance decreased during infusion of acetylcholine by 28% and 25% in the off-pump and on-pump groups. After surgery the decrease was 16% and 6% respectively (p=0.028 and p<0.001, compared to preoperative response). The response did not differ between the two groups before, but did so after surgery (p=0.01). Saline had no effect. Conclusion: The better maintained endothelium-dependent vasodilatation in the off-pump group indicated less endothelial dyfunction.77 Nine patients with stable angina pectoris subjected to off-pump surgery and 18 patient subjected to on-pump surgery (nine patients with stable angina and nine with unstable angina), received acetylcholine (10 microgr.) and adenosine (18 microgr.) given as bolus into a vein-graft anastomosed to a coronary vessel. The blood flow in the vein-graft (i.e. indirectly the flow in the targeted coronary circulation) and hemodynamic were observed. In the off-pump group, acetylcholine evoked an increase with +14 +/- 12% of control in coronary blood flow, while in the stable on-pump group, acetylcholine decreased the blood flow with –60 +/- 8% of baseline and in the unstable on-pump group the flow was decreased with –38 +/- 8% of baseline. Between the stable on- and off-pump groups, no significant difference. Adenosine significantly increased the coronary blood flow in all three groups with +81 +/- 14% in the off-pump patients; with 95 +/- 14% in the stable on-pump group and with +74 +/- 13% in the unstable on-pump group. Neither acetylcholine nor adenosine injection caused any changes in hemodynamic.Conclusion: On-pump coronary bypass surgery appears to be more harmful to the coronary endothelium, in terms of acetylcholine-induced vasoconstriction, compared to off-pump surgery. Furthermore, there is no significant difference in direct smooth muscle vascular reactivity between off-pump and on-pump cornary bypass surgery. No apparent dissimilarities in endothelial dysfunction were observed in the stable and unstable on-pump groups suggesting other causes for differences in post-operative outcome for these patients.78 |
|
|
|
Literature: |